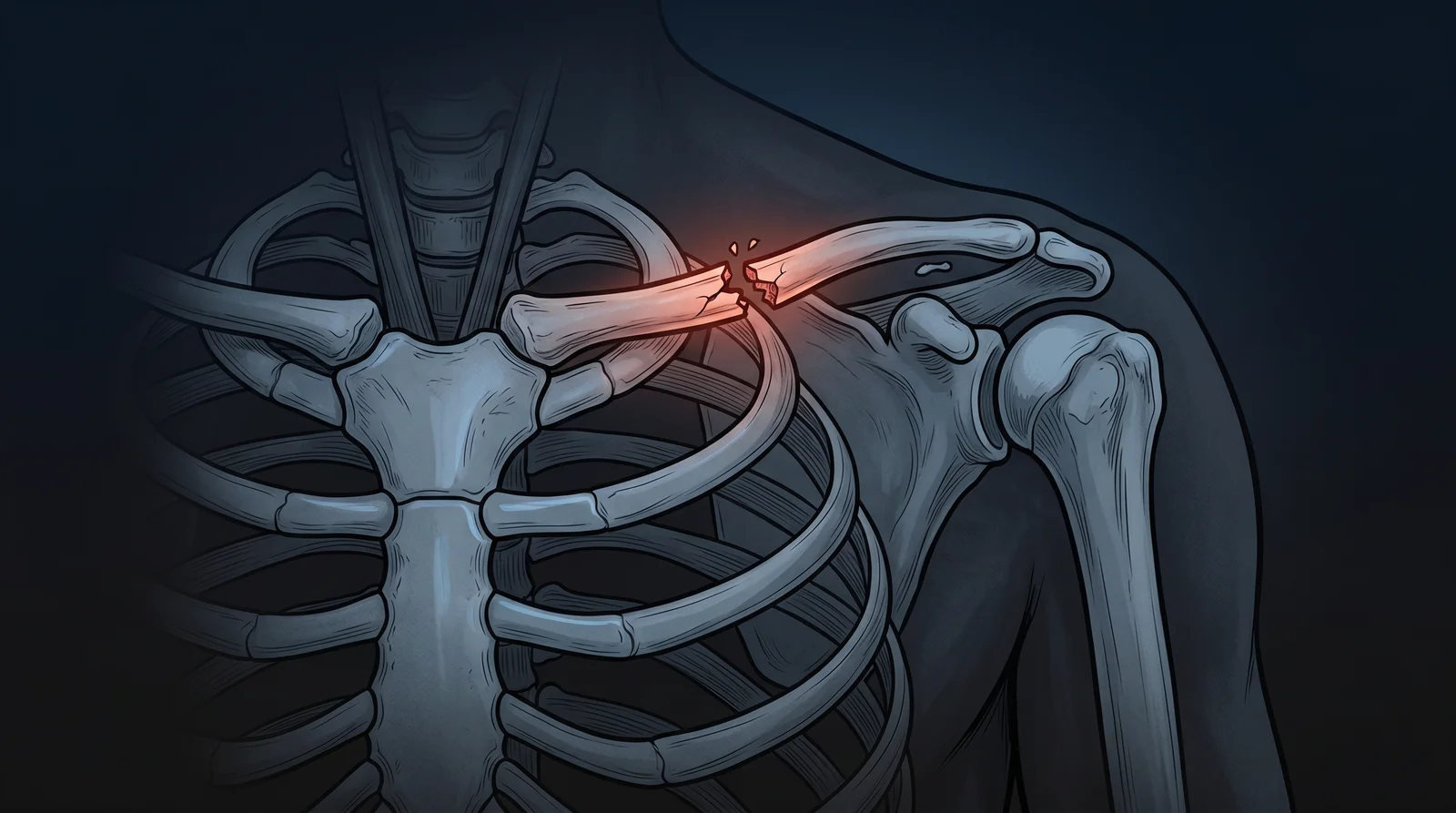
Clavicle Fracture From a Car Accident
A clavicle fracture is a break in the collarbone, the narrow S-shaped bone that links your breastbone to your shoulder blade. It is the most commonly broken bone in adults, accounting for roughly 2.6 to 4 percent of all adult fractures according to a StatPearls review published through the National Library of Medicine. In a Kentucky car crash, the break usually comes from the seat belt loading diagonally across the chest, a direct side impact to the shoulder, or a fall on an outstretched hand when the car finally stops. Whether it heals cleanly or leaves you with permanent weakness depends on how far the fragments moved, what imaging you get, and what happens in the first two to three weeks.
Table of Contents Show
- 1. What a Clavicle Fracture Actually Is
- 2. How a Car Accident Breaks the Clavicle
- 3. Symptoms and Red Flags
- 4. Why the Emergency Room Sometimes Gets It Wrong
- 5. The Imaging That Confirms the Diagnosis
- 6. Treatment Timeline: Non-Surgical vs. Surgical
- 7. Long-Term Complications To Watch For
- 8. Residual Impairment Ratings and Functional Limitations
- 9. The Insurance Defense Playbook
- 10. Documentation Strategy
- 11. Kentucky PIP, Statute of Limitations, and the Two-Year Clock
- 12. What To Do Next
What a Clavicle Fracture Actually Is
The clavicle is the narrow, gently curved bone you can feel running from the base of your neck out to the tip of your shoulder. It is the only bone that ties your arm to the rest of your skeleton. Every time you reach, lift, push, or pull, force travels through it. A break there changes almost everything you do with your upper body.
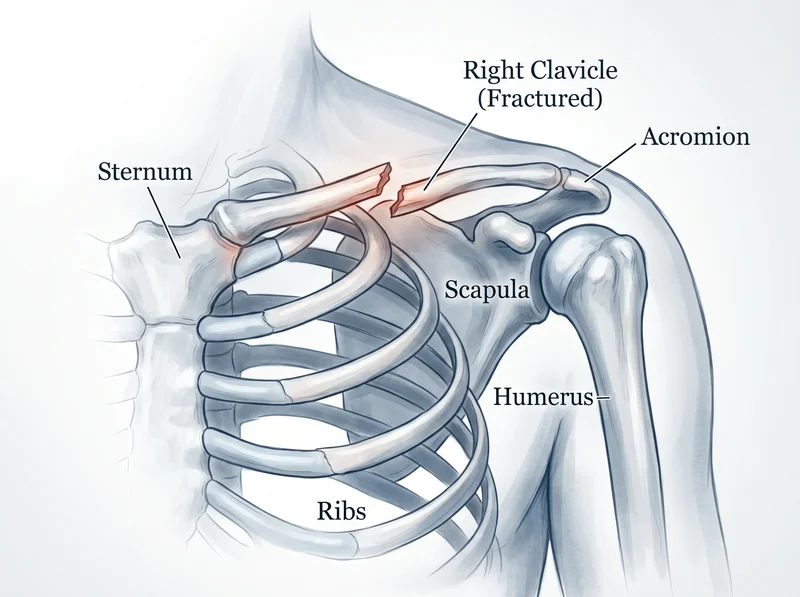
Orthopedic surgeons split the clavicle into three zones. The middle third is where roughly 69 to 82 percent of fractures happen, according to the American Academy of Orthopaedic Surgeons. The distal (lateral) third, closest to the shoulder, accounts for about 15 to 20 percent and is the hardest to heal because strong ligaments pull the two fragments apart. The medial third, closest to the sternum, is rare but serious because the bone sits directly over the subclavian vein, the subclavian artery, and the top of the lung.
Beyond the zone, surgeons care about three things: how far the fragments moved (displacement), whether the bone shortened (shortening), and how many pieces it broke into (comminution). The Robinson classification, also called the Edinburgh classification and published in the Journal of Bone and Joint Surgery, sorts fractures by those three features. Whether your fracture is Robinson Type 2B1 or 2B2 is the difference between a sling and a plate. That is not a decision you make. It is a decision your orthopedic surgeon makes from your imaging, and one the insurance company will later try to second-guess.
How a Car Accident Breaks the Clavicle
In a Kentucky crash, clavicle fractures almost always come from one of four loading patterns. Each one sends force through the bone in a direction it was not built to handle.
- Seat belt loading across the chest. In a frontal collision, the shoulder belt loads diagonally from your opposite hip up to the same-side shoulder. At crash speeds, that belt can apply thousands of pounds of force over a few tenths of a second. The middle third of the clavicle, which has no muscular or ligament support along most of its length, bows and snaps. The National Highway Traffic Safety Administration includes seat-belt-related clavicle and sternum fractures in its list of common thoracic injury patterns.
- Direct impact to the shoulder. In a side-impact or T-bone crash, the door pushes into the shoulder at the point of the acromion. Force drives inward along the axis of the clavicle. The bone fails somewhere between the acromion and the sternum, usually in the lateral or middle third. These impacts are often comminuted and often require surgery.
- Fall on an outstretched hand (FOOSH). When the car spins or rolls, occupants throw an arm out to catch themselves against the door, the pillar, or the window. Force travels up the arm, through the shoulder, and into the clavicle. This is the same mechanism that breaks collarbones in cyclists and skiers. It is common after rollovers and after partial ejections.
- Airbag and door-column contact in rollover events. During a rollover, occupants bounce inside the cabin and contact the window sill, the door frame, or the roof rail. The clavicle is often the first bone to absorb that load because it sits at the outer edge of the shoulder. Complex and comminuted fractures are more common in these crashes than in any other.
One more pattern shows up in rear-end crashes, especially when the driver has a death grip on the steering wheel. The clavicle braces against the forward-forceful motion of the torso, and the bone fails under that leverage. This pattern turns up repeatedly in clients who hit the steering wheel or shoulder belt hard after a hard rear-impact at highway speed.
Symptoms and Red Flags
Most people know something is wrong with the collarbone within seconds. The ones who do not are usually distracted by a head injury, chest pain, or adrenaline. Here is what the pain pattern looks like.
Sharp pain directly over the collarbone
Press one finger along the top of the collarbone. A fracture hurts sharply at a single point and often feels like a grinding sensation under the skin.
A visible bump or tenting of the skin
Displaced fragments often push a bump up through the skin. In thinner patients the bone can look like it is trying to poke through the skin. That is an urgent surgical flag.
The shoulder droops forward and down
Without the clavicle holding the shoulder back, the weight of the arm pulls the shoulder forward. The injured side sits lower than the other.
Cannot lift the arm above shoulder height
Lifting the arm requires the clavicle to rotate. When the bone is broken, the arm locks out at about 60 to 90 degrees of elevation.
A grinding or crunching feeling
Clinicians call this crepitus. It is the sound of two broken bone ends rubbing together. It confirms a fracture and rules out a simple contusion.
Numbness or tingling down the arm
The brachial plexus, the bundle of nerves that powers your arm, runs right under the clavicle. A displaced fragment can press on or stretch those nerves. Numbness down the arm is a red flag that belongs in the emergency room the same hour.
Red flags that mean emergency room now, not tomorrow.
Skin tenting from a sharp fragment, pale or cold fingers on the injured side, numbness or weakness in the hand, difficulty breathing, or a palpable step-off at the sternum all mean urgent evaluation. Rare but real complications include pneumothorax, subclavian vessel injury, and brachial plexus injury. Do not wait for a same-day urgent care slot for any of these.
Why the Emergency Room Sometimes Gets It Wrong
Emergency rooms diagnose clavicle fractures well. Where they fall short is on the classification that drives treatment. A typical ER workup is a front-back (AP) X-ray of the shoulder and a discharge paper that says clavicle fracture, sling, follow up with orthopedics. That is correct but incomplete.
The problem is displacement. A single AP X-ray is not enough to measure how far the fragments have moved or how much the bone has shortened. Many patients end up in a sling for weeks, watching a displaced fracture drift further out of position, before an orthopedic surgeon finally orders the right views and realizes the window for a clean repair is closing. By that point, callus has started to form, and the decision is harder.
Two imaging details matter. A Zanca view tilts the beam 15 degrees upward and shows the distal third clearly. A Serendipity view tilts the beam 40 degrees upward and shows the medial third. Without those, medial and distal fractures can look almost normal on a standard film. A CT scan is the gold standard for comminuted or medial third fractures because it shows the three-dimensional pattern the surgeon actually has to fix.
The Imaging That Confirms the Diagnosis
Getting the right imaging early is the single most important step after a crash-related collarbone injury. The diagnostic hierarchy looks like this.
- AP and cephalic tilt X-rays. Standard AP shows the middle third. A Zanca view (15 degrees cephalic tilt) shows the distal third. A Serendipity view (40 degrees cephalic tilt) shows the medial third. You need at least two views to measure displacement accurately.
- Weight-bearing or upright X-rays. Gravity pulls the shoulder down and reveals ligament injuries around the distal clavicle (acromioclavicular joint disruption) that lying-down films hide. A paper in the Journal of the American Academy of Orthopaedic Surgeons notes that non-weight-bearing films routinely underestimate displacement.
- CT scan with 3D reconstruction. For comminuted fractures, medial third fractures, or any fracture that looks like it may need surgery, a CT gives the surgeon a map of the fragment pattern. It also rules out pneumothorax and first rib fracture, which often travel with high-energy clavicle injuries.
- CT angiography. Ordered when pulses are diminished on the injured side or when the mechanism suggests subclavian vessel injury. Rare but life-saving when indicated.
- MRI. Not routinely needed for the fracture itself, but used when rotator cuff tears, labral tears, or brachial plexus injury are suspected alongside the fracture.
Every client who contacts Sam Aguiar Injury Lawyers after a clavicle fracture has imaging reviewed by our medical team. If the right views are missing, we get them. If an orthopedic referral is slow, we push it up. Imaging is the foundation of the medical record your case is built on.
Treatment Timeline: Non-Surgical vs. Surgical
For decades, nearly every clavicle fracture was treated in a sling. In the last twenty years, orthopedic literature has shifted. Large randomized trials, including a multicenter trial published in the Journal of Bone and Joint Surgery, showed that completely displaced mid-shaft clavicle fractures heal better when they are plated than when they are left in a sling. Surgery is no longer the rare option. It is the right call for a specific subset of fractures.
Non-Surgical Treatment
Non-surgical care works well for minimally displaced fractures (less than 100 percent translated), fractures with less than 2 centimeters of shortening, and fractures with no neurovascular threat. The typical path:
| Stage | Timing | What Happens |
|---|---|---|
| Sling | Week 0 to 2 | Simple arm sling, sometimes a figure-of-eight brace. Ice, anti-inflammatories, avoid lifting anything heavier than a coffee mug. |
| Gentle motion | Week 2 to 6 | Pendulum exercises. Passive range of motion starts around week 4. Repeat X-ray confirms the fragments are not drifting. |
| Active motion | Week 6 to 12 | Sling comes off around week 6. Active range of motion and light strengthening. Callus is visible on X-ray. |
| Strength and return | Month 3 to 6 | Formal physical therapy. Return to work for desk jobs by week 4 to 6. Return to heavy labor by month 3 to 4. |
| Final healing | Month 6 to 12 | Bone remodels. Final imaging confirms union. A minority of patients develop a painful bump at the fracture site that may need later excision. |
Surgical Treatment (ORIF)
Open reduction and internal fixation (ORIF) means the surgeon opens the skin, reduces the fragments back into anatomical position, and holds them there with a metal plate and screws. For completely displaced mid-shaft fractures, for most comminuted fractures, and for unstable distal third fractures, this is the modern standard of care.
| Stage | Timing | What Happens |
|---|---|---|
| Surgery | Week 0 to 3 | Outpatient ORIF, 60 to 90 minutes under general anesthesia. Plate placed on the superior or anterior surface. |
| Sling | Week 0 to 2 | Arm in a sling for comfort. Pendulum exercises begin within a few days. |
| Range of motion | Week 2 to 6 | Active-assisted range of motion. Most patients are back to desk work within 1 to 2 weeks. Driving resumes around week 3 to 4. |
| Strength | Week 6 to 12 | Formal physical therapy. Gradual return to lifting. Heavy lifting and contact activity usually wait until week 12. |
| Hardware | Month 12+ | Plates are often left in place permanently. Some patients request removal if the plate is prominent under the skin. |
Surgery gets people back to work and back to full shoulder function sooner. The scar is usually 3 to 4 inches long. Plate prominence is a real but manageable side effect. Non-surgical care avoids the incision but has a higher rate of malunion and nonunion in truly displaced fractures, and a longer return to heavy lifting.
“When I was hit, I knew who to call. Sam and his team took care of all my needs and handled everything! I am so thankful.”— E. Cooper
Long-Term Complications To Watch For
Even a well-treated clavicle fracture can leave a footprint. The long-term complications that matter most to a personal injury claim are these.
- Malunion. The bone heals but in the wrong position. Shortening of more than 2 centimeters leaves a visible deformity, reduced shoulder strength, and chronic aching. A Robinson series in the Journal of Bone and Joint Surgery linked greater than 2 cm of shortening to increased rates of patient-reported dissatisfaction.
- Nonunion. The bone does not heal. Incidence is roughly 15 percent for displaced mid-shaft fractures treated without surgery, based on multiple pooled series. Nonunion often requires a bone graft plus plate fixation later.
- Shoulder weakness and winged scapula. Loss of clavicle length changes how the scapula sits on the chest wall. The shoulder blade wings out and overhead strength drops measurably on dynamometer testing.
- Brachial plexus irritation. A displaced fragment or exuberant callus can press on the nerves and cause numbness, tingling, and weakness in the hand. Thoracic outlet syndrome is a recognized late complication in a small subset of patients.
- Hardware prominence. The plate sits directly under thin skin. In slim patients it can be uncomfortable under shoulder straps or backpacks. Removal is a second surgery.
- Post-traumatic arthritis of the acromioclavicular (AC) joint. Distal third fractures often disturb the AC joint and lead to arthritis years later. That is why distal fractures are handled differently by most shoulder surgeons.
Residual Impairment Ratings and Functional Limitations
When a clavicle fracture does not heal to full function, the gap between where you were before the crash and where you are now becomes a documented, measurable impairment. Orthopedic surgeons use the AMA Guides to the Evaluation of Permanent Impairment to assign a whole-person impairment rating. That number affects your life in two concrete ways: it tells the insurance adjuster there is permanent damage, and it tells a jury precisely how much shoulder function you lost.
The Guides rate shoulder impairment primarily on range of motion and strength. Typical post-clavicle-fracture deficits that generate an impairment rating include reduced forward flexion (inability to fully lift the arm overhead), reduced abduction (inability to reach sideways), and grip or shoulder-strength loss on dynamometer testing. A physician who only examines you in the office, without a full functional capacity evaluation, will routinely understate your impairment.
Return-to-activity milestones matter as much as the impairment rating itself. The American Academy of Orthopaedic Surgeons describes a graduated progression from pendulum exercises at week two through full-resistance lifting at month three for uncomplicated cases. When a patient cannot reach those milestones on schedule, every delayed milestone should be documented in the medical record. Delayed milestones and a below-normal functional capacity at maximum medical improvement form the backbone of a permanent-impairment argument.
Why impairment ratings matter in a Kentucky crash case.
A documented whole-person impairment rating from a board-certified orthopedic surgeon transforms a “broken collarbone that healed” narrative into a measurable permanent loss. Insurance adjusters routinely dismiss shoulder injuries as temporary. An impairment rating puts a peer-reviewed number on what you actually lost.
For clients who do physical work, the impairment rating often translates directly to reduced earning capacity. A roofer who cannot fully elevate the arm overhead after a displaced clavicle fracture cannot do the core movements of the job. A physical therapist or occupational therapist can produce a formal functional capacity evaluation that documents work restrictions. That report becomes part of the medical record your case is built on.
The Insurance Defense Playbook
Once the at-fault driver’s insurance company learns there is a clavicle fracture in a crash, the claim file gets handed to an adjuster who has seen thousands of them. The adjuster’s job is to pay as little as possible. Their playbook looks like this.
- Minimize the injury. “Clavicle fractures heal fine in a sling.” That line shows up in almost every first offer. The adjuster ignores displacement, shortening, nonunion risk, and hardware prominence. The response is a written demand package with the full imaging record, the operative report when applicable, and a letter from the treating surgeon on why this fracture is not the easy kind.
- Push for a recorded statement. “Just routine, this helps us document the claim.” A recorded statement taken three days after the crash, before imaging confirms displacement or pneumothorax, becomes an anchor the insurance company uses for the rest of the case. Do not give one without an attorney on the line.
- Demand an early medical authorization. A broad medical authorization lets the adjuster pull ten years of records and mine them for anything that looks like a pre-existing shoulder problem. A hobby injury from 2014 becomes the new cause of the 2026 fracture. Narrow, time-limited authorizations scoped to the treatment the crash caused are the right response. See our page on pre-existing conditions and Kentucky crash claims for how this plays out.
- Blame the seat belt. “The belt saved your life but also caused the fracture, so it is really the belt’s fault.” The seat belt is not a legal defense. The at-fault driver caused the crash that caused the belt to load. Adjusters do not get to rewrite basic tort law.
- Make a lowball offer at 45 days. The offer lands before surgery, before final imaging, and sometimes before the client is off the sling. Settling early, before maximum medical improvement, is the single most expensive decision a Kentucky crash victim can make.
- Delay, delay, delay. Every phone call unreturned, every document “still in review,” is an economic strategy. Adjusters who miss response deadlines get a litigation hold letter and a call from an attorney with Forbes honors and a Trucking Trial Lawyers Association Top 10 record.
Documentation Strategy
The medical record you build in the weeks after a Kentucky clavicle fracture determines how much the insurance company takes the claim seriously. Gaps in that record, missed appointments, undocumented symptoms, imaging not ordered, become arguments the adjuster uses against you. Here is how to build a record that holds up.
Imaging cadence
AP X-ray at ER. Zanca and Serendipity views at first orthopedic visit. Repeat AP at week 2 to 4 to confirm or deny fragment drift. CT if surgical planning is needed. Final imaging at maximum medical improvement. Each study should have a written radiology read in the file.
Orthopedic visit notes
Every visit note should document current range of motion measurements in degrees, strength testing results, and a comparison to the prior visit. Vague notes like “doing well, continue sling” are useless for a claim. Ask for specific measurements and get copies.
Physical therapy records
PT records show the gap between what your shoulder could do before therapy started and what it can do at discharge. Each session note documents a pain level, a range of motion measurement, and a functional goal met or missed. Those records tell the story of your recovery arc.
Functional capacity evaluation
An FCE, performed by an occupational therapist or physical therapist, documents exactly what physical tasks you can and cannot perform at maximum medical improvement. For workers with physical jobs, this is the most important document in the file.
Daily symptom log
A short written log, even one sentence per day, of what you could not do because of the injury: could not lift a laundry basket, could not drive, could not sleep on the injured side. Juries remember specifics, not adjectives. Start the log the day of the crash and keep it until the case closes.
Employer and wage records
Pay stubs for the 12 months before the crash, your employer’s time-off letter documenting missed days, and any modified-duty restrictions imposed by your surgeon. For self-employed clients, tax returns for the prior two years plus bank statements documenting the income drop.
Bigger Share Guarantee®
You will always walk away from your Kentucky clavicle fracture case with more than the firm does, after medical liens, litigation costs, and fees. If your share is ever less than ours, we cut our fee. That is not a slogan. It is the rule we measure every case by.
$0 Out-Of-Pocket ForeverKentucky PIP, Statute of Limitations, and the Two-Year Clock
Kentucky is a choice no-fault state. Most drivers carry Personal Injury Protection (PIP, also called Basic Reparation Benefits), a first-party coverage that pays medical bills, lost wages, and replacement services up to $10,000 per person per accident. PIP is supposed to pay those bills quickly, without a fight about fault.
Kentucky’s statute of limitations for a motor vehicle crash is found in KRS 304.39-230. It runs two years from the last PIP payment or two years from the date of the accident, whichever is later. That is longer than most people think, but you cannot count on the PIP carrier keeping the clock open by paying late bills. Every clavicle fracture case in our office gets a statute-of-limitations date locked in at intake.
One more PIP rule catches people. Kentucky allows certain drivers to reject PIP by filing a rejection form. If you or the at-fault driver rejected PIP, the medical bill rules change. That is not a do-it-yourself research project. Call us and let us pull the coverage records.
What To Do Next
If you or someone in your household has a suspected or confirmed clavicle fracture after a Kentucky car crash, the order of operations below gives you the best shot at a clean recovery and a complete case record.
- Confirm the imaging. Ask the ER or your primary care provider for AP, Zanca, and Serendipity views of the clavicle. If the fracture is comminuted or the films are ambiguous, request a CT scan.
- Get in front of an orthopedic surgeon within 2 weeks. That is the window where displaced fractures can still be plated cleanly. Past 3 weeks, the decision becomes harder.
- Document the daily impact. Keep a short log of what you cannot do: lift a laundry basket, drive to work, pick up a child, sleep on the injured side. Juries and adjusters remember specifics, not adjectives.
- Do not sign an insurance company medical authorization. Do not give a recorded statement. Refer the adjuster to your attorney or to our office.
- Save everything. Crash photos, ambulance report, ER paperwork, discharge summary, X-ray and CT images on disc, surgeon notes, physical therapy notes, pharmacy records, pay stubs, and any time-off letter from your employer. We will organize the record. You just need to keep it.
- Call Sam Aguiar Injury Lawyers. We will walk through your imaging, pull the crash report, confirm coverage, and start the Bigger Share Guarantee clock. No cost, no pressure.
Internal Resources for Kentucky Crash Victims
A clavicle fracture rarely travels alone. Here are the related pages our injury team updates most often.
- Car Accident Injuries Hub for every injury category we handle.
- Shoulder Injuries for rotator cuff, labrum, and AC joint injuries that often pair with clavicle fractures.
- Rotator Cuff Tear From a Car Accident for the soft tissue injury that often hides alongside a clavicle fracture.
- Scaphoid Fracture From a Car Accident for wrist fractures from the same outstretched-hand mechanism that breaks many collarbones.
- Pre-Existing Conditions and Kentucky Crash Claims for how we address the old-injury argument.
- Radiology and Imaging in Injury Claims for how imaging drives the medical record that drives the case.
Frequently Asked Questions
How do I know if my collarbone is really broken, or just bruised?
Sharp pain directly over the clavicle, a grinding or crunching feeling when you move the shoulder, a visible bump or sagging of the shoulder, and trouble lifting the arm above shoulder height are the classic signs. A plain X-ray confirms it. Bruises hurt over a wider area, do not grind, and do not keep you from raising the arm. The American Academy of Orthopaedic Surgeons recommends X-ray for any suspected clavicle injury after trauma.
Do all clavicle fractures need surgery?
No. Minimally displaced middle-third fractures with less than 2 centimeters of shortening usually heal well in a sling. Completely displaced fractures, comminuted fractures, unstable distal third fractures, and fractures with skin tenting or neurovascular threat are the ones that are plated. An orthopedic surgeon makes the call after reviewing the imaging, per guidance from the National Library of Medicine.
How long does it take to recover from a clavicle fracture after a car accident?
Non-surgical healing takes roughly 6 to 12 weeks for bone union and 3 to 6 months for full function. ORIF patients often return to desk work within 1 to 2 weeks and regain full shoulder strength by month 4. Heavy labor and contact activity typically wait until month 3 to 4. Real-world recovery is slower for older patients and for smokers, according to the AAOS.
Should I give a recorded statement to the at-fault driver’s insurance company?
No. Kentucky law does not require you to give one to the other driver’s insurance company. Recorded statements are used as anchors against you later, especially when they are taken before your imaging is complete and your diagnosis is confirmed. Tell the adjuster to contact your attorney. If you do not have one, call us before you say anything on record.
Can I still have a case if I was wearing my seat belt and the seat belt caused the fracture?
Yes. The seat belt is not a legal defense. The at-fault driver caused the crash. The belt loaded across your body because the crash happened. Kentucky law compensates for the injury the crash caused, and that includes the fracture the belt created while it was saving your life. Wearing the belt almost always strengthens a case, not weakens it.
What is the statute of limitations for a clavicle fracture case in Kentucky?
Under KRS 304.39-230, the statute of limitations for a Kentucky motor vehicle crash is two years from the date of the accident or two years from the last PIP payment, whichever is later. Do not assume a later PIP payment saved your claim. Lock the date in with an attorney at intake.
What if the fracture was missed or misclassified by the ER?
It happens more than people think. Medial and distal third fractures do not show well on a standard AP X-ray. If you left the ER with a normal report but the pain, grinding, and functional loss continue, request a repeat film with dedicated Zanca and Serendipity views and ask for an orthopedic referral. A missed fracture is not the end of the claim. It becomes part of the medical record we document.
Does PIP cover clavicle fracture treatment after a Kentucky car accident?
Yes, if you carry PIP (Basic Reparation Benefits). Kentucky is a choice no-fault state, so PIP is optional, but most drivers keep it. PIP covers medical bills, lost wages, and replacement services up to $10,000 per person regardless of who caused the crash. If PIP was rejected by you or the at-fault driver, the coverage rules change. See KRS 304.39-230 for the statutory framework.
Does Sam Aguiar Injury Lawyers charge anything up front?
No. $0 Out-Of-Pocket Forever. We front every cost, from medical record retrieval to expert witnesses to depositions. Our fee comes out of the recovery at the end, and under the Bigger Share Guarantee®, you always walk away with more than the firm. If that math ever fails, we cut our fee.

