On This Page
Post-traumatic stress disorder (PTSD) is a recognized psychiatric diagnosis under the DSM-5-TR that can develop after a car crash involves perceived life threat, sympathetic nervous system activation, and disrupted memory consolidation in the hippocampus and amygdala. According to the National Institute of Mental Health, PTSD is documented in approximately 20% of motor vehicle accident survivors. In Kentucky, psychological injuries do not automatically fall within no-fault PIP coverage under KRS 304.39-060 and require medical records meeting the tort threshold to pursue the at-fault driver. Diagnosis is confirmed through clinical interview using the CAPS-5 and the PCL-5 self-report checklist. Evidence-based treatments include Prolonged Exposure (PE), Cognitive Processing Therapy (CPT), and EMDR.
How Common Is PTSD After Car Crashes
Motor vehicle crashes are the leading civilian cause of PTSD in the United States. A 2025 systematic review and meta-analysis published in Health Promotion Perspectives pooled data across studies and found that PTSD prevalence among road traffic accident survivors reaches 29.4% at one month post-crash, decreasing to 18.8% at three months as some individuals recover naturally, and stabilizing near 20% for those with chronic presentations. Longitudinal research published in Behaviour Research and Therapy tracked accident survivors three years post-crash and found that 11% still met full diagnostic criteria, with those scoring high on symptom severity at one year having a 53%–72% probability of persistence at year three.
These numbers matter in Kentucky for a practical reason: insurance adjusters treat psychological injury claims as inherently weaker than fracture or surgical claims. The medical science does not support that assumption. PTSD is a diagnosable, measurable, and treatable neuropsychiatric condition with structural brain correlates confirmed by functional MRI. Understanding the biology is the first step in demonstrating that this injury is as real and as documentable as a broken bone.
Neuroanatomy of Trauma
PTSD is not a personality weakness or an emotional reaction. It is a disorder of neurological dysregulation in specific, identifiable brain structures. According to research summarized by Michigan State University’s Foundations of Neuroscience, three regions are consistently altered in individuals with PTSD: the amygdala, the hippocampus, and the prefrontal cortex. Each plays a distinct role in why crash survivors continue to experience fear, fragmented memories, and hyperreactivity long after the physical danger is over.
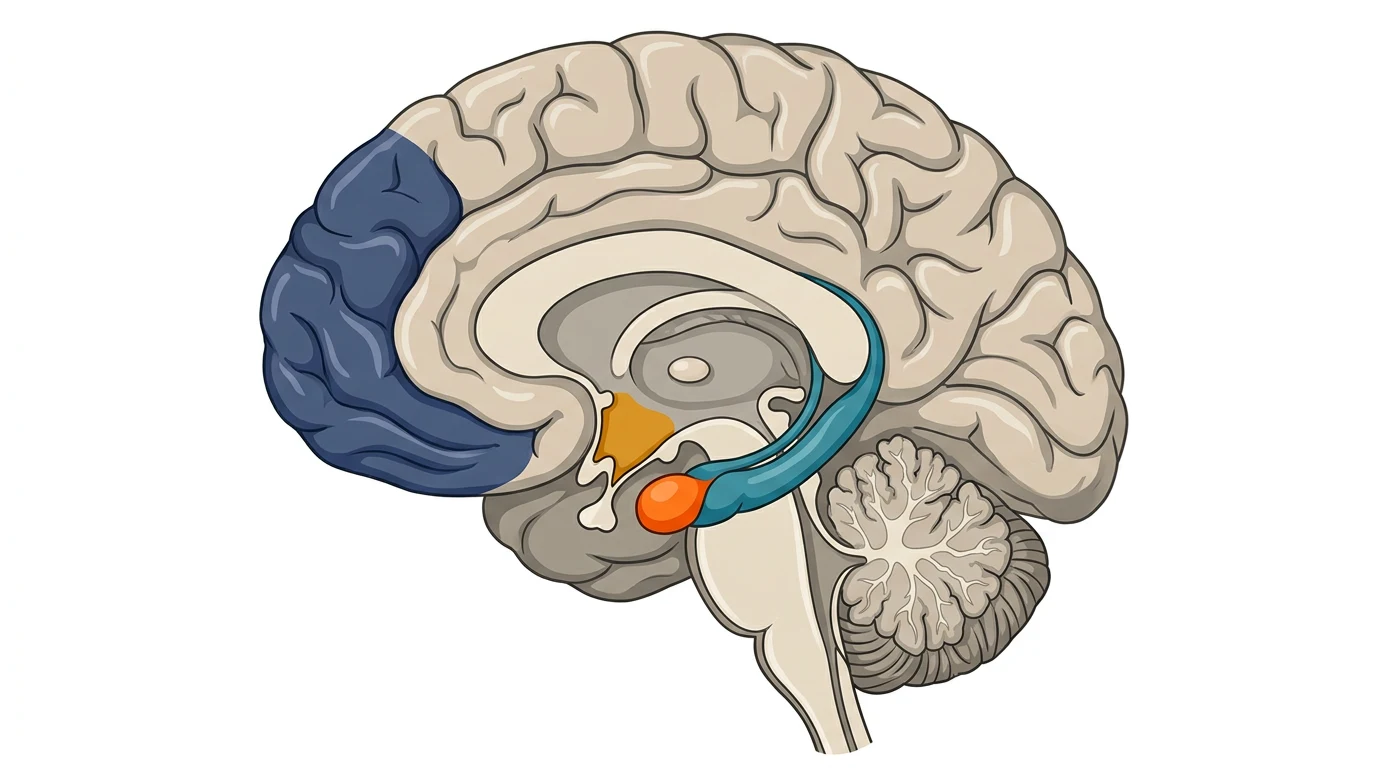
Amygdala: Brain’s Threat Detector
The amygdala sits in the medial temporal lobe and functions as the brain’s primary threat-detection and fear-encoding center. In a healthy stress response, it fires, triggers the sympathetic alarm cascade, and then quiets as the threat passes. In PTSD, the amygdala becomes hyperactivated and hypersensitive, continuing to fire in response to non-threatening stimuli that resemble any aspect of the original crash—the sound of brakes, a glimpse of a stopped vehicle in traffic, the smell of gasoline. Published neuroimaging studies in Depression and Anxiety (PMC3233765) consistently demonstrate elevated amygdala metabolic activity in PTSD compared to trauma-exposed individuals without PTSD.
Hippocampus: Context and Memory Center
The hippocampus encodes episodic memory and, crucially, assigns temporal context to experiences—placing them in the past rather than the present. In PTSD, hippocampal function is compromised and hippocampal volume is reduced. A longitudinal volumetric study published in Molecular Psychiatry found that smaller right hippocampus volume at time of acute trauma was associated with a non-remitting PTSD trajectory. When the hippocampus fails to contextualize a traumatic memory as past, the brain experiences that memory as happening now—which explains why flashbacks are not “remembering” in the ordinary sense but a neurological reliving.
Prefrontal Cortex: The Regulator
The ventromedial prefrontal cortex (vmPFC) normally acts as a top-down regulatory brake on amygdala reactivity. In PTSD, vmPFC activity is reduced, meaning the brake is weaker. As documented in a peer-reviewed analysis in the Journal of Experimental and Basic Medical Sciences, this reduced vmPFC inhibition leaves the amygdala firing unchecked. The functional result is emotional dysregulation, impaired threat assessment, and the intrusive symptom cluster central to PTSD.
HPA Axis: Cortisol Regulation
The hypothalamic-pituitary-adrenal (HPA) axis is the body’s primary hormonal stress system. Under normal circumstances, the HPA axis releases cortisol in response to threat and then returns to baseline. Research published in Frontiers in Psychiatry documents that in PTSD, HPA axis regulation becomes chronically disrupted—both the amygdala and hippocampus lose their normal modulating influence over cortisol release. The result is sustained physiological stress even in the absence of any real threat, contributing to sleep disturbance, cardiovascular strain, immune dysfunction, and the fatigue that pervades the daily lives of PTSD survivors.
How a Car Crash Creates PTSD
Not every traumatic experience becomes PTSD. Three mechanisms, identified in research from the National Institute of Mental Health and the VA National Center for PTSD, are particularly relevant to motor vehicle crashes.
Perceived Life Threat
The DSM-5-TR Criterion A requires exposure to actual or threatened death or serious injury. In a high-speed collision, the brain processes the event as a life-threatening emergency whether or not the physical injuries are severe. The perceived life threat—not the objective injury severity—activates the sympathetic cascade. This is why a crash victim with relatively minor physical injuries can develop significant PTSD while someone with more severe injuries may not: what matters neurologically is how the brain interpreted the threat in the moment.
Sympathetic Nervous System Activation
At the moment of impact, the sympathetic nervous system fires instantaneously. Heart rate spikes, pupils dilate, blood flow shunts to large muscles, and stress hormones flood the bloodstream. This is the biological survival response. Under ordinary circumstances, it resolves after the threat passes. In vulnerable individuals, the sympathetic system does not fully deactivate. The crash survivor remains in a partial state of alarm—hypervigilant, easily startled, unable to relax in cars or near intersections. This prolonged activation is the physiological substrate of the hyperarousal cluster in PTSD.
Memory Consolidation Failure
During extreme stress, elevated cortisol and catecholamines interfere with the hippocampus’s normal process of organizing and “closing” traumatic memories. Instead of being encoded as a coherent narrative that can be placed in the past, the crash memory fragments into disconnected sensory shards—a flash of headlights, the sound of screeching tires, the smell of airbag deployment. These fragments cannot be integrated into ordinary autobiographical memory. They intrude unbidden as flashbacks or intrusive images. This failure of memory consolidation, documented extensively in PTSD neuroscience literature, is the neurological explanation for why time does not simply “heal” PTSD on its own.
DSM-5-TR Diagnostic Criteria
PTSD is diagnosed under the American Psychiatric Association’s DSM-5-TR criteria (Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition, Text Revision). Eight criteria must be met. In a personal injury context, each criterion corresponds to medical documentation that establishes the diagnosis as clinically legitimate and causally connected to the crash.
Exposure to actual or threatened death, serious injury, or sexual violence—directly experienced, witnessed, or learned about happening to a close person. A car crash meets this criterion when the survivor experienced perceived life threat.
One or more intrusion symptoms: recurrent distressing memories, nightmares, flashbacks (dissociative re-experiencing), or intense psychological or physiological distress at cues resembling the crash.
Persistent avoidance of internal memories and thoughts about the crash, or external reminders such as driving, intersections, vehicles, or passengers.
Negative alterations in cognition and mood: inability to recall crash details, exaggerated negative beliefs about oneself or the world, persistent guilt, diminished interest in activities, emotional numbing, inability to experience positive emotions.
Marked alterations in arousal and reactivity: irritable outbursts, hypervigilance, exaggerated startle response, concentration problems, sleep disturbance, reckless or self-destructive behavior.
Duration exceeds one month; symptoms cause clinically significant distress or functional impairment; symptoms are not attributable to substances or another medical condition.
Dissociative and Delayed Presentations
Two DSM-5-TR specifications are clinically important in crash cases. First, the dissociative subtype applies when the individual experiences depersonalization (feeling detached from oneself) or derealization (surroundings feel unreal) in addition to standard PTSD criteria. Second, the delayed expression specifier applies when full diagnostic criteria are not met until at least six months after the crash—meaning PTSD can be legitimately diagnosed well after the accident date with no gap in causation.
Diagnostic Tools: PCL-5 and CAPS-5
Two validated instruments are used to assess PTSD, and both are directly relevant to building a documentation record for an injury claim.
PCL-5: The PTSD Checklist for DSM-5
The PCL-5, developed and validated by the VA National Center for PTSD, is a 20-item self-report measure in which the patient rates each DSM-5 symptom on a 0–4 scale of severity over the past month. Total scores range from 0 to 80. Initial research suggests a cutoff score of 31–33 is indicative of probable PTSD. The PCL-5 is used to screen for probable PTSD, quantify symptom severity, and track treatment progress over time. In a claims context, PCL-5 scores obtained at multiple points provide objective, serially dated documentation of symptom severity—something an adjuster cannot dismiss as merely subjective.
CAPS-5: The Gold Standard Diagnostic Interview
The Clinician-Administered PTSD Scale for DSM-5 (CAPS-5) is a 30-item structured clinical interview conducted by a trained mental health clinician. It is, as the VA states, the gold standard for diagnosing PTSD. The CAPS-5 assesses both frequency and intensity of each DSM-5 criterion symptom, yielding a total severity score that supports or rules out diagnosis. When a forensic psychiatrist or psychologist retained by the defense challenges your diagnosis, a documented CAPS-5 evaluation from a treating clinician with multiple sessions of contact with the patient carries far more weight than a one-time independent medical examination (IME) conducted by the defense’s hired evaluator.
Differential Diagnosis: What PTSD Is Not
Accurate diagnosis requires distinguishing PTSD from related conditions. Misdiagnosis in either direction hurts the crash victim—underdiagnosis leaves an injury undocumented; overdiagnosis or misclassification gives the defense a target to attack.
Acute Stress Disorder (ASD)
ASD is diagnosed when a PTSD-symptom cluster appears within three days of a traumatic event and lasts between three days and one month. If symptoms persist beyond one month, the diagnosis converts to PTSD. This distinction matters for claim documentation: a treating provider who notes ASD in the immediate post-crash period and then documents the transition to PTSD at the one-month mark establishes a clear clinical narrative of how the disorder evolved.
Adjustment Disorder
Adjustment disorder involves emotional or behavioral symptoms in response to a stressor, but it does not require the specific intrusion, avoidance, negative cognition/mood, and hyperarousal clusters of PTSD. Insurance adjusters and defense IME physicians sometimes attempt to reclassify PTSD as the less severe “adjustment disorder” to minimize the clinical significance of the diagnosis. The rebuttal is the CAPS-5 evaluation: the structured clinical interview applies DSM-5 criteria systematically and produces a symptom severity score that either meets or does not meet the PTSD threshold.
Mild Traumatic Brain Injury (mTBI) Overlap
This overlap is particularly common in crash cases. Both PTSD and mTBI cause memory deficits, concentration problems, sleep disturbance, irritability, and emotional dysregulation. In a crash with airbag deployment, sudden deceleration, or head contact, both conditions can coexist. Treating providers must assess both independently. The existence of traumatic brain injury does not exclude a concurrent PTSD diagnosis, but a defense expert may attempt to attribute all symptoms to mTBI to avoid the psychiatric injury claim. Neuropsychological testing and structured psychiatric evaluation by separate specialists, documented in the medical record, addresses this challenge directly.
Why Misdiagnosis Damages the Claim
If a treating provider documents only “anxiety” or “adjustment disorder” without conducting a formal PTSD evaluation, the insurance company treats the psychological injury as transient and minor. The medical record becomes the primary battleground in a Kentucky injury claim. Gaps in the diagnostic record—not gaps in the symptoms—are what adjusters exploit. A treating psychiatrist or psychologist who completes the CAPS-5, documents serial PCL-5 scores, and provides a narrative connecting each DSM-5 criterion to the crash is building the clinical foundation that any competent plaintiff’s attorney needs.
Objective Evidence: Imaging and Biomarkers
One of the most powerful arguments against the “PTSD is just subjective” defense position is the growing body of objective measurement available. None of these measures are used to diagnose PTSD clinically—diagnosis remains clinical, using DSM-5-TR criteria and structured interviews. But in litigation, objective biomarkers rebut the adjuster’s claim that the injury cannot be measured.
fMRI Findings
Functional MRI studies consistently show two characteristic patterns in PTSD: amygdala hyperactivation in response to threat-related stimuli, and hippocampal volume reduction compared to trauma-exposed controls without PTSD. A large-cohort study published in the Archives of General Psychiatry (PMC3647246) found that PTSD diagnosis was associated with statistically significant smaller left and right amygdala volume and smaller left hippocampal volume after controlling for depression, alcohol use, intracranial volume, and trauma load. fMRI is not routinely ordered as part of standard PTSD care, but when forensic neuroimaging is obtained by a treating specialist, results consistent with PTSD pathology constitute powerful objective evidence in a legal proceeding.
Heart Rate Variability (HRV)
Heart rate variability measures the variation in time intervals between heartbeats and reflects the balance between sympathetic and parasympathetic nervous system activity. Research documents reduced HRV in PTSD, reflecting the persistent sympathetic activation and impaired autonomic regulation described above. HRV can be measured non-invasively during a clinical visit using standard ECG equipment. Serial HRV measurements, combined with clinical documentation, provide a physiological record of the dysregulation that persists in untreated or undertreated PTSD.
Salivary Cortisol
Salivary cortisol reflects HPA axis activity and stress hormone levels. Research reviewed in Frontiers in Psychiatry documents that PTSD is associated with chronic HPA axis dysregulation, with cortisol patterns that deviate from healthy stress-and-recovery cycles. As a non-invasive biomarker, salivary cortisol collected at standardized times (morning awakening, evening) and across multiple days provides objective evidence of HPA dysregulation that can be presented to a trier of fact as a measurable physiological correlate of the psychological injury.
Kentucky Expert Testimony: KRE 702 and Daubert
Any expert who testifies about PTSD neuroimaging, HRV, or cortisol in a Kentucky court must meet the admissibility standard under Kentucky Rule of Evidence 702. Kentucky follows the Daubert standard—not Frye. Under KRE 702, expert testimony is admissible when it is based on sufficient facts or data, is the product of reliable principles and methods, and the expert has reliably applied those methods to the facts of the case. Peer-reviewed fMRI research, published in indexed journals, conducted by credentialed researchers, and applied by a qualified forensic psychiatrist or neurologist to the specific patient’s documented history meets this standard. The defense’s Daubert challenge to such evidence can be addressed by showing the underlying research has been peer-reviewed, published, and is generally accepted in the relevant scientific community.
Evidence-Based Treatment
The 2023 VA/DoD Clinical Practice Guideline for PTSD Management represents the most authoritative evidence-based treatment recommendations available. The guideline prioritizes psychotherapy over pharmacotherapy and identifies three trauma-focused psychotherapies as strongly recommended.
Prolonged Exposure (PE)
Prolonged Exposure is a manualized cognitive-behavioral protocol developed at the University of Pennsylvania. It involves imaginal exposure—detailed verbal recounting of the traumatic event—and in-vivo exposure to avoided situations in real life. The VA/DoD CPG recommends PE with a typical course of 8–15 individual sessions, each 90 minutes long. PE is specifically designed to disrupt the avoidance that maintains PTSD: by repeatedly and safely confronting the traumatic memory and avoided triggers, the amygdala’s conditioned fear response extinguishes over time. For car crash survivors who have stopped driving, avoid intersections, or cannot tolerate being a passenger, PE is directly applicable to the injury-caused limitations that affect daily life and earning capacity.
Cognitive Processing Therapy (CPT)
Cognitive Processing Therapy targets the “stuck points”—distorted beliefs that developed as a result of the trauma, such as “I caused the crash,” “I can never be safe,” or “I am permanently damaged.” The standard CPT protocol is 12 sessions, either individual or group. CPT is particularly effective for the Criterion D symptom cluster: negative alterations in cognition and mood. For crash survivors who carry guilt, shame, or catastrophic beliefs about the future, CPT addresses the cognitive distortions that can make standard exposure work difficult to engage.
EMDR (Eye Movement Desensitization and Reprocessing)
EMDR uses bilateral sensory stimulation (typically eye movements) while the patient briefly focuses on traumatic memories. The VA/DoD CPG recommends EMDR with a typical course of 6–12 sessions. The exact mechanism is debated in the research literature, but outcomes data consistently place EMDR on par with PE and CPT for PTSD reduction. EMDR is often preferred when the patient finds imaginal or verbal exposure approaches difficult to tolerate.
Pharmacotherapy: FDA-Approved Medications
Two medications have FDA approval specifically for PTSD: sertraline (Zoloft) and paroxetine (Paxil), both selective serotonin reuptake inhibitors (SSRIs). The 2023 VA/DoD CPG endorses both, as well as venlafaxine (an SNRI), as appropriate pharmacological options, typically used in combination with psychotherapy rather than as standalone treatment. For nightmare suppression—a particularly disruptive symptom in motor vehicle crash survivors—the VA/DoD CPG identifies prazosin, an alpha-1 adrenergic blocker, as having evidence for reducing PTSD-related nightmares, though it is not FDA-approved for this indication.
Recovery Timeline by Phase
Recovery from post-crash PTSD follows a phased clinical trajectory. Understanding these phases matters both for treatment planning and for documenting the injury’s impact across time for a claim.
PTSD Phase Timeline After a Car Crash
- Acute Phase (0–1 month): Symptoms emerge. Meets criteria for Acute Stress Disorder (ASD) during this window. Key intervention: early psychological first aid, safety planning, initial psychiatric evaluation. Not all individuals with ASD develop PTSD—some resolve naturally within this window.
- Subacute Phase (1–3 months): If symptoms persist beyond one month, PTSD diagnosis is established. This is the optimal window to begin PE, CPT, or EMDR—earlier treatment is associated with better outcomes. PCL-5 screening at this stage establishes a documented baseline severity score.
- Chronic Phase (3+ months): PTSD that persists beyond three months is classified as chronic. Functional impairment in this phase—inability to drive, return to work, maintain relationships—is well-documented in peer-reviewed literature as permanent or semi-permanent without structured treatment.
- Complex or Refractory Phase: When standard first-line treatments (PE, CPT, EMDR) have not produced adequate symptom reduction after two or more treatment trials, the condition may be classified as complex or treatment-resistant PTSD. This presentation requires specialist-level care, may involve medication augmentation, and carries a more guarded long-term functional prognosis. In a claim, refractory PTSD supported by a documented treatment history and specialist opinion establishes serious, ongoing impairment.
“I was in a crash that left me afraid to drive for months. Sam’s team took me seriously from day one. They understood that what I was going through was a real injury, not just nerves. I’m grateful every day that I made that call.”
Insurance Defense Playbook
Insurance carriers defending PTSD claims from car crashes deploy a predictable set of tactics. Knowing them in advance is the best preparation.
Tactic 1: The “Pre-Existing Anxiety” Attack
The adjuster orders a records review and finds any prior mental health treatment—a therapy appointment from years before the crash, an anxiety prescription, a counseling note. The argument: your PTSD was there before the crash; the accident did not cause it.
Tactic 2: “Subjective Complaint” Minimization
The adjuster characterizes PTSD as “self-reported symptoms” with no objective basis—implying exaggeration or fabrication. This tactic is particularly common when the physical injuries appear minor on imaging.
Tactic 3: The IME with a Defense-Selected Forensic Psychiatrist
The carrier sends the claimant to an independent medical examination (IME) conducted by a forensic psychiatrist they select and pay. These examiners review records, conduct a one-time clinical interview, and frequently produce reports that minimize or deny the PTSD diagnosis.
Tactic 4: Surveillance and Social Media Mining
Investigators document the claimant driving a car, attending a social event, or posting photographs that suggest normal activity. The argument: if you have PTSD, why were you at a birthday party?
Tactic 5: Treatment Gap Exploitation
Adjusters flag any gap between appointments—a missed session, a period without treatment—as evidence that the injury was not serious or was resolved.
Tactic 6: Causation Challenge—Apportionment to Pre-Crash Stressors
The defense’s forensic psychiatrist opines that the claimant’s symptoms are primarily caused by life stressors unrelated to the crash—work, finances, relationship difficulties—rather than the motor vehicle accident.
Kentucky-Specific Legal Framework
Kentucky No-Fault PIP and Psychological Injury
Kentucky is a choice no-fault state under KRS 304.39-060. Personal Injury Protection (PIP) provides up to $10,000 in basic reparations benefits for medical expenses and lost wages following a crash, without regard to fault. However, PIP coverage under standard Kentucky policies historically has not automatically covered mental health and psychiatric treatment as primary medical expenses in the same way as physical injuries. The applicable medical treatment must be causally connected to the crash, and psychiatric treatment claims are subject to carrier review and potential denial.
Critically, to bring a tort claim against the at-fault driver for pain and suffering—which encompasses PTSD impairment—the injured party must either (a) have incurred more than $1,000 in medical expenses, (b) have suffered a bone fracture, permanent disfigurement, or permanent injury, or (c) have rejected the no-fault limitation by opting out of PIP before the crash. Psychiatric treatment costs counted toward the $1,000 threshold strengthen the ability to pursue the at-fault driver. Detailed medical bills, treatment records, and provider statements connecting PTSD treatment to the crash are the foundation.
Proving Permanent Impairment
Chronic or refractory PTSD that produces persistent functional impairment—inability to return to driving, reduced earning capacity, ongoing psychiatric care dependency—may meet the “permanent injury” threshold independently of the $1,000 medical expense requirement. A treating psychiatrist or psychologist who provides a written opinion that the PTSD meets the standard for permanent psychiatric impairment, using criteria from the AMA Guides to the Evaluation of Permanent Impairment or the life care planning framework, creates the clinical foundation for this argument.
KRE 702 and Expert Admissibility
Kentucky Rule of Evidence 702 governs the admissibility of expert testimony in state court proceedings. Kentucky follows the Daubert standard, requiring that expert testimony be based on sufficient facts or data, employ reliable methodology, and apply that methodology reliably to the case-specific facts. A forensic psychiatrist testifying about PTSD diagnosis, causation, treatment, and prognosis must be prepared to withstand a Daubert hearing. Peer-reviewed diagnostic criteria (DSM-5-TR), validated psychometric instruments (CAPS-5, PCL-5), and published neuroimaging research provide the scientific foundation that satisfies KRE 702.
Internal Resources for Kentucky Crash Victims
PTSD does not exist in isolation after a car crash. It frequently co-occurs with physical injuries and requires coordinated medical and legal management. The following resources on our site address related aspects of Kentucky crash injury claims:
- Traumatic Brain Injury after a Car Crash — mTBI and PTSD frequently overlap; separate diagnoses and documentation are critical
- Anxiety After a Car Accident — distinguishing generalized anxiety from PTSD and Acute Stress Disorder
- Kentucky No-Fault PIP Coverage — how PIP interacts with psychiatric injury claims and the tort threshold
- Kentucky Tort Threshold Explained — what your medical records must establish to pursue the at-fault driver
- Life Care Planning for Crash Injuries — documenting long-term psychiatric care needs for chronic PTSD
Documentation Strategy: Building the Clinical Record
The medical record is the primary asset in a Kentucky PTSD claim. Everything the treating provider writes—and everything they fail to write—will be reviewed by the adjuster, the defense attorney, and potentially a jury. Here is the documentation framework that creates the strongest foundation.
Immediate Post-Crash Documentation
Seek psychiatric or psychological evaluation within the first two to four weeks after the crash. At that initial evaluation, the provider should document the crash event and the patient’s subjective account of perceived life threat; the presence and severity of all DSM-5-TR criterion symptoms; a PCL-5 score as a baseline; the provisional ASD or PTSD diagnosis; and the proposed treatment plan. This establishes temporal proximity from the first clinical encounter.
Ongoing Treatment Records
Serial PCL-5 scores at each appointment create a quantitative timeline of the disorder’s progression or response to treatment. Session notes should document functional impairment specifically: “Patient reports inability to drive on interstate; has declined two work projects requiring out-of-town travel.” These specifics translate into concrete evidence of how PTSD has altered the person’s daily life and earning capacity.
CAPS-5 Evaluation
Request a formal CAPS-5 evaluation from the treating clinician or a consulting specialist. The CAPS-5 results, preserved in the medical record with the total severity score and criterion-by-criterion findings, provide the gold standard diagnostic documentation that preempts the defense’s characterization of PTSD as merely “self-reported.”
Pre-Crash Medical Records
Obtain your complete pre-crash psychiatric and primary care records. If those records show no prior PTSD diagnosis, no prior trauma-related treatment, and stable functioning before the accident date, they are powerful evidence of causation. Do not wait for the defense to subpoena them—review them first with your attorney.
Frequently Asked Questions
Can I claim PTSD without a physical injury from the car crash?
Yes. PTSD can develop from a crash even when physical injuries are minor or not apparent on imaging. The DSM-5-TR Criterion A requires only that the person was exposed to actual or threatened death or serious injury—the perceived life threat during the crash is sufficient, regardless of whether a fracture or surgical injury occurred. A formal psychiatric diagnosis, documented with CAPS-5 and PCL-5 records, establishes the psychological injury independently of physical findings. Kentucky tort law does not require physical injury as a prerequisite for a psychiatric injury claim.
What evidence proves PTSD from a car crash?
The strongest evidence package combines: (1) a treating psychiatrist or psychologist’s diagnosis using DSM-5-TR criteria; (2) a CAPS-5 structured clinical interview with documented severity score; (3) serial PCL-5 self-report scores from multiple treatment visits; (4) clinical notes documenting functional impairment across driving, work, and relationships; (5) temporal proximity established through pre-crash and post-crash medical records; and (6) absence of prior PTSD diagnosis in pre-crash records. Objective biomarker data—HRV measurements, salivary cortisol profiles, or forensic neuroimaging—can supplement the clinical record when the defense challenges the diagnosis aggressively.
How do I document PTSD for my injury claim?
Start with a psychiatric or psychological evaluation within the first month after the crash—the sooner the better to establish temporal proximity. Ask your treating provider to administer the PCL-5 at each visit and document the score in the chart. Request that a formal CAPS-5 be completed and preserved in your medical record. Keep a daily journal noting symptoms, triggers, and specific functional impacts such as missed work days, avoided driving routes, or cancelled activities. Collect all pre-crash mental health records so your attorney can establish the baseline before the crash.
Does Kentucky no-fault PIP cover PTSD treatment costs?
Kentucky PIP (basic reparations benefits under KRS 304.39-060) covers medical expenses causally related to the crash up to the $10,000 basic limit. Psychiatric and psychological treatment costs—therapy sessions, psychiatric medication management, CAPS-5 evaluations—are medical expenses that may be submitted to PIP. However, carriers often scrutinize mental health claims and may require documentation linking each treatment to the crash injury. Your treating provider’s clinical notes and diagnostic documentation are essential for PIP reimbursement. Additionally, those psychiatric treatment costs count toward the $1,000 medical expense threshold required to pursue the at-fault driver in tort.
Can I be diagnosed with PTSD without a head injury?
Absolutely. PTSD is a psychiatric disorder caused by psychological trauma, not brain tissue injury. Head contact, loss of consciousness, and traumatic brain injury are entirely separate diagnoses. A crash victim who perceived life threat during the collision—regardless of whether they struck their head—meets Criterion A of the DSM-5-TR and can develop PTSD. The neurological changes in PTSD—amygdala hyperactivation, hippocampal volume reduction—occur through neurochemical and neuroplastic mechanisms driven by the stress response, not through direct physical brain trauma.
What if PTSD symptoms do not appear right away after the crash?
The DSM-5-TR includes a “delayed expression” specifier: full diagnostic criteria may not be met until at least six months after the traumatic event, even though some symptoms appear immediately. This means PTSD diagnosed months after a crash is clinically legitimate and can still be causally connected to that crash event. Delayed onset does not weaken the claim; it is a recognized and documented clinical presentation. What matters is thorough documentation when symptoms do appear, establishing the connection between current symptoms and the prior crash through detailed clinical history.
What is the difference between the PCL-5 and the CAPS-5?
The PCL-5 is a 20-item self-report questionnaire completed by the patient, scoring each DSM-5 PTSD symptom from 0 to 4. A total score of 31–33 or higher indicates probable PTSD. It is used for screening and tracking symptom severity over time across multiple visits. The CAPS-5 is a 30-item structured clinical interview administered by a trained mental health professional—the gold standard for PTSD diagnosis according to the VA National Center for PTSD. In an injury claim, the CAPS-5 carries greater weight because it was administered by a clinician and cannot be characterized as mere self-report.
Will the defense’s IME doctor say I do not have PTSD?
Defense IME physicians are paid by the insurance carrier, see the claimant once, and review records supplied by the defense. Their reports often minimize or deny PTSD diagnoses. The strongest countermeasure is a treating provider with a long, well-documented clinical relationship—multiple visits, serial PCL-5 scores, a completed CAPS-5—versus a one-time IME. Under Kentucky Rule of Evidence 702, the defense IME methodology can be challenged at deposition and at a Daubert hearing: ask how many sessions the IME physician spent with the claimant, whether they administered the CAPS-5, and what peer-reviewed basis they used to conclude the DSM-5-TR criteria were not met.
How long does PTSD treatment take after a car crash?
First-line psychotherapy protocols have defined durations: Prolonged Exposure typically runs 8–15 sessions; Cognitive Processing Therapy is 12 sessions; EMDR is typically 6–12 sessions. Many patients achieve meaningful symptom reduction within these timeframes when treatment begins early. Chronic and refractory presentations—those that persist beyond three months without adequate treatment response—may require extended treatment, medication augmentation, or specialist-level care. The clinical prognosis and realistic treatment duration are part of the documentation picture that informs the functional impact of the injury across the full period of impairment.


