Seatbelt Injuries in Kentucky Car Accidents
On This Page
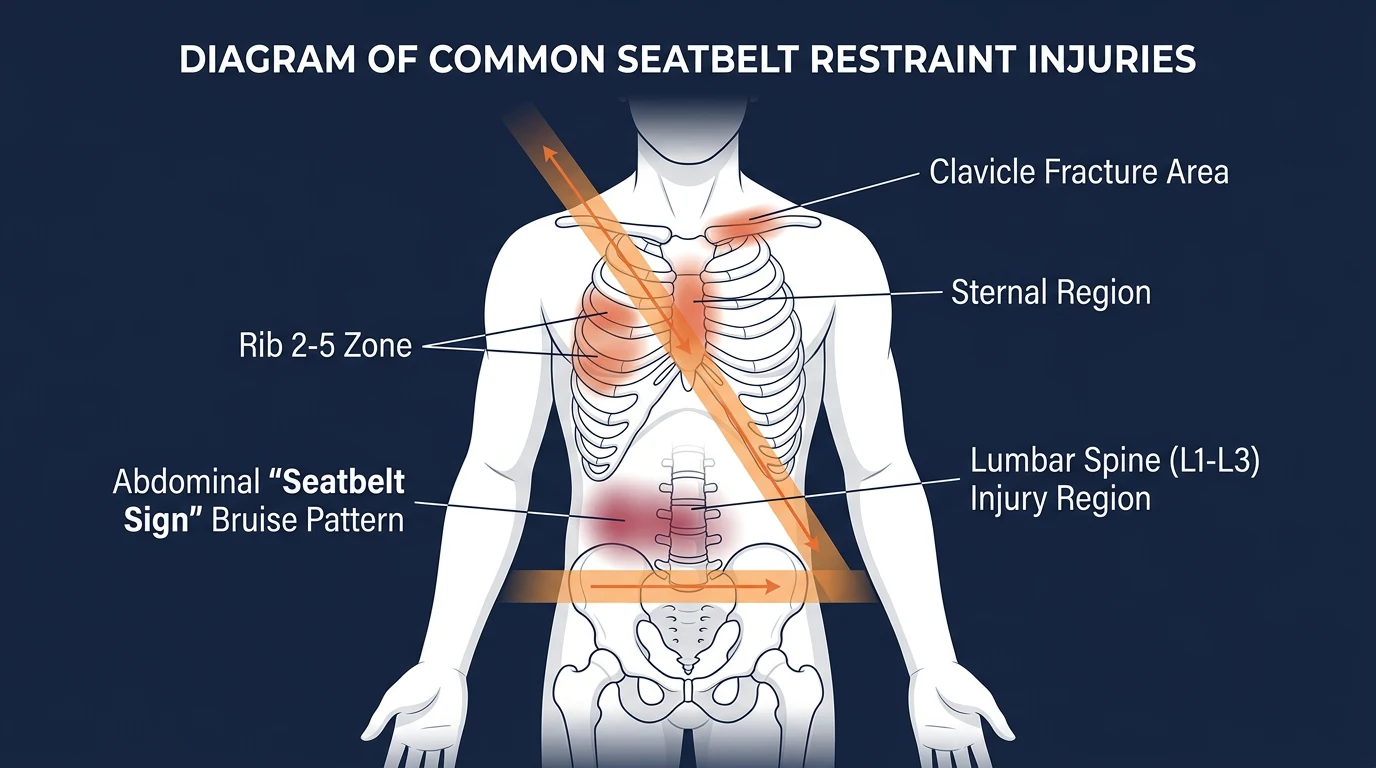
Seatbelts save lives, but in high-force collisions they also cause a predictable set of injuries: clavicle fractures, sternal and rib fractures, Chance fractures of the lumbar spine (L1–L3), abdominal organ tears, and small bowel perforations. The visible bruise left by a seatbelt, called the seatbelt sign, correlates with internal injury in roughly 30% of cases and is treated as objective evidence of impact force. Kentucky law under KRS 189.125 requires seatbelt use. If the seatbelt caused your injuries, you still have a full claim against the at-fault driver. Sam Aguiar Injury Lawyers handles seatbelt injury cases across Kentucky with $0 out-of-pocket forever.
How Seatbelts Cause Injuries: The Physics
Modern vehicles use a three-point restraint system: a diagonal sash strap that runs from the shoulder across the chest, and a lap belt that crosses the pelvis. During a frontal or side collision, the occupant decelerates at rates that can exceed 30 g-forces in less than 200 milliseconds. The seatbelt arrests that deceleration by distributing force across the chest wall, the clavicle, the sternum, and the pelvis.
The sash strap concentrates force along a narrow band from the left clavicle across the right lower ribs. The lap belt applies a localized pressure bar across the lower abdomen and the upper pelvic rim. Research published in the Bulletin of Emergency and Trauma documents that three-point belts are specifically associated with clavicle fractures, sternal fractures, rib fractures, and hollow viscus injuries, while older two-point lap-only belts concentrate force across the lower back and abdomen.
Two specific failure modes amplify injuries in three-point systems:
Restraint Failure Patterns
- Submarining: The pelvis slides forward under the lap belt, so the belt rides up over the abdomen instead of the pelvic rim. This concentrates belt force directly on soft abdominal organs and the lumbar spine rather than the bony pelvis. Submarining dramatically increases the rate of bowel perforation and lumbar spine fractures.
- Seatbelt syndrome (belt syndrome): The specific constellation of abdominal seatbelt sign combined with lumbar Chance fracture and bowel or mesenteric injury. First described in the medical literature in 1962, belt syndrome is the most serious sequela of restraint-associated injury patterns.
According to NHTSA data, seatbelts reduce the risk of fatal injury to front-seat passenger car occupants by 45%. The same forces that save lives in severe crashes are those that cause the injuries documented below.
Anatomy of Seatbelt Injury Patterns
Seatbelt injuries follow predictable anatomic distributions based on which belt component contacts which body region. Understanding this anatomy is essential for proper injury mechanism documentation.
Shoulder and Chest Wall Injuries (Sash Strap)
The diagonal sash strap transmits the largest decelerative force. Structures in the strap's path absorb this energy in a consistent sequence:
Clavicle (Collarbone): The clavicle is the first bony structure the sash contacts. Mid-shaft fractures are the most common pattern, classified by Robinson's classification (Type 2B1 and 2B2 are the displaced fractures most often requiring surgery). Because the clavicle articulates with both the sternum medially and the acromioclavicular (AC) joint laterally, displaced fractures can disrupt both joints. See our detailed clavicle fracture page for full anatomy, classification, and treatment options.
Sternum: The sternum (breastbone) absorbs the medial sash force. Sternal fractures are graded by their transverse location: manubrium (upper segment), body, or xiphoid process. A sternal fracture is not "soft tissue" injury. CT imaging of the chest in the ER frequently demonstrates displaced sternal body fractures that carry a risk of associated cardiac contusion, aortic injury, and pneumothorax. The Abbreviated Injury Scale (AIS) for the chest grades these injuries from AIS 2 (minor) to AIS 5 (critical).
Ribs 1–12: The sash strap crosses ribs 2–5 on the contralateral side (right ribs for a driver with a left-shoulder sash). As documented in RadioGraphics (RSNA), chest abrasions from the belt are associated with sternal and rib fractures and injuries to the heart and thoracic aorta. Multiple rib fractures (two or more ribs in two or more places) produce a "flail segment" that may require surgical stabilization. Even single rib fractures cause severe pain, impair respiration, and require aggressive pulmonary toilet (breathing exercises, incentive spirometry, and sometimes epidural analgesia) to prevent pneumonia during recovery.
Cervical Spine and Soft Tissue: The sash strap contacts the neck during forward flexion. Neck abrasions from seatbelt contact are specifically associated with carotid artery injury, laryngeal fracture, and cervical spine fractures. Cervical injury severity can be classified with the Spence criteria for atlas fractures and the AO/Magerl classification for subaxial injuries. Soft-tissue cervical strain following a seatbelt-restrained crash is not the same as whiplash. The force vector is different, the structures loaded are different, and MRI for ligamentous injury is indicated when plain films and CT are negative but symptoms persist.
Abdominal and Lumbar Injuries (Lap Belt)
The lap belt applies a direct compression load across the lower abdomen. At high velocity, this compressive force has two consequences: it drives the abdominal organs backward against the rigid lumbar spine, and it serves as the axis of rotation when the upper body continues to flex forward.
Chance Fracture (L1–L3 Lumbar Spine): First described by British radiologist G.Q. Chance in 1948, the Chance fracture is a flexion-distraction injury in which the lap belt acts as the fulcrum, subjecting the entire posterior spinal column to tension forces. Research published in the American Journal of Roentgenology documents that Chance-type fractures are associated with intra-abdominal injury in 40% of cases. The fracture propagates as a horizontal line through the vertebral body, pedicles, transverse processes, laminae, and spinous process. The Magerl/AO Classification designates these as Type B1 injuries (transosseous tension band disruption). Lumbar spine injuries of this pattern require urgent CT with reconstructions, and unstable cases require surgical stabilization.
Small Bowel and Mesenteric Injury: The small bowel (jejunum and ileum) and its mesenteric blood supply are the structures most vulnerable to direct compression between the lap belt and the lumbar vertebrae. Bowel perforation can be occult on initial CT and may only become apparent 6–12 hours later as peritoneal signs develop. The Eastern Association for the Surgery of Trauma (EAST) practice management guidelines specify that patients with seatbelt sign and abdominal tenderness must be admitted for serial physical examination because CT sensitivity for hollow viscus injury is imperfect.
Solid Organ Injuries: The spleen and liver can sustain lacerations from the combined effects of compression and deceleration. Splenic capsular tears, liver lacerations, and even diaphragmatic rupture have been reported in association with belt syndrome in published case series.
Injury Pattern by Belt Type
- Three-point (shoulder + lap): Clavicle fracture, sternal fracture, ribs 2–5, cervical soft tissue, hollow viscus injury, splenic laceration
- Lap-only (older vehicles, rear seats): Chance fracture L1–L3, bowel perforation, mesenteric tear, abdominal wall disruption
- Submarining (improper routing): Amplifies all abdominal and lumbar injury patterns regardless of belt type
The Seatbelt Sign as Evidence
The seatbelt sign is a bruise, abrasion, or ecchymotic marking on the skin that follows the exact path of the seatbelt. It is both a clinical finding and a medicolegal exhibit.
From a medical standpoint, Radiopaedia documents that a positive abdominal seatbelt sign combined with abdominal pain or tenderness significantly increases the likelihood of intra-abdominal injuries. The RadioGraphics systematic review established that skin abrasions of the neck, chest, and abdomen indicate internal injury in 30% of cases. The sign should prompt a diligent search for related injuries across all involved anatomic regions.
Seatbelt Sign Evidence
In a Kentucky injury claim, the seatbelt sign does three things that benefit your position:
- It establishes restraint use. Under KRS 189.125, seatbelt use is mandatory in Kentucky. A seatbelt sign photographed at the ER proves you were wearing your belt. This eliminates the most common insurance defense tactic: attacking you for non-compliance.
- It establishes force vector. The diagonal pattern of the bruise identifies whether it was the sash (chest/shoulder) or lap belt (abdomen) that generated the injury, helping radiologists and surgeons identify what to look for on imaging.
- It creates objective documentation. Unlike subjective pain complaints, the seatbelt sign is a photograph taken by hospital staff. It cannot be argued away, minimized by an Independent Medical Examiner (IME), or recharacterized by defense counsel as pre-existing.
If you were seen in the ER or urgent care after a crash, your medical records should include nursing documentation and photographs of any seatbelt sign. If your treating providers did not photograph it, do so yourself immediately after any crash. The bruise pattern fades within 5–10 days and cannot be reproduced later.
ER Imaging Protocol for Seatbelt Injuries
Seatbelt injuries are routinely underdiagnosed at the initial ER visit because the force distribution creates injuries across multiple body regions simultaneously. A complete imaging workup following a positive seatbelt sign should include the following studies:
Standard Imaging Sequence
If your ER evaluation stopped at a chest X-ray and you were sent home, and you subsequently developed worsening back pain, abdominal pain, or neurological symptoms, return to the ER immediately. Bowel perforation and unstable Chance fractures can have delayed presentations.
Treatment: Conservative vs. Surgical Management
Treatment decisions for seatbelt injuries depend on injury severity, stability, and the presence of neurological compromise. Each injury type has a distinct management pathway.
Clavicle Fractures
Conservative: Non-displaced or minimally displaced mid-shaft fractures are treated with a figure-8 harness or simple sling immobilization for 4–6 weeks, followed by progressive range-of-motion exercises. Conservative management is appropriate for Robinson Type 2A fractures with less than 2 cm shortening.
Surgical (ORIF): Displaced fractures (Robinson Type 2B1 and 2B2) with significant shortening, comminution, or neurovascular compromise are treated with open reduction and internal fixation. Two approaches are available: (1) Plate fixation using a 3.5mm anatomical locking plate applied to the superior or anteroinferior surface of the clavicle, or (2) Intramedullary (IM) rod fixation using a titanium elastic nail (TENS nail) inserted through the medial clavicle. Research published in the Malaysian Orthopaedic Journal demonstrates equivalent functional outcomes for both techniques at 24 weeks, with IM nailing offering shorter hospital stays. See our clavicle fracture treatment guide for full surgical decision criteria.
Sternal and Rib Fractures
Conservative: Most sternal fractures and isolated rib fractures are managed non-operatively with pain control, pulmonary toilet (incentive spirometry, deep breathing exercises, coughing), and monitoring for associated cardiac contusion or pneumothorax. Pain management is critical because uncontrolled pain causes splinting (shallow breathing) that leads to atelectasis and pneumonia.
Surgical: A traumatic pneumothorax or hemothorax requires chest tube placement (tube thoracostomy). Flail chest with respiratory compromise may require surgical rib fixation using titanium plates or U-clips applied to the fractured ribs. Chest injury management at a Level I trauma center is strongly recommended when multiple rib fractures are present.
Lumbar Chance Fractures
Conservative: Stable Chance fractures (purely osseous, no ligamentous disruption, no neurological deficit) in appropriate candidates can be managed with a thoracolumbosacral orthosis (TLSO) brace and physiotherapy for 10–12 weeks. The AO Foundation designates these as Type B1 injuries with excellent healing potential.
Surgical: Unstable Chance fractures with ligamentous disruption (Type B2/B3), neurological deficit, gross instability, or concurrent bowel injury require operative stabilization. The standard approach is posterior open reduction and internal fixation with pedicle screw and rod constructs placed one level above and below the fracture. AO Foundation surgical references document the posterior short-segment fixation technique as the standard of care. Minimally invasive percutaneous cannulated pedicle screw systems (MIS approach) offer equivalent stability with reduced surgical morbidity for selected patients. A posterior midline approach is used to expose the fractured level, decompress the spinal canal if needed, and place instrumentation. Fusion with bone graft is added for highly unstable injuries. Lumbar spine injury recovery following surgical fixation requires intensive physical and occupational therapy beginning within the first weeks after surgery.
Abdominal and Bowel Injuries
Gastric decompression with nasogastric tube placement is the first-line intervention for suspected bowel injury. Bowel perforations require exploratory laparotomy with primary repair or bowel resection and anastomosis. Mesenteric tears with active hemorrhage require ligation or embolization. Solid organ injuries (spleen, liver) are graded by the American Association for the Surgery of Trauma (AAST) organ injury scale and managed from observation (Grade I–II) to splenorrhaphy, angioembolization, or splenectomy (Grade III–V) depending on hemodynamic status. Internal organ injuries following motor vehicle crashes demand Level I trauma center management.
Recovery Timeline by Phase
Seatbelt injury recovery is not linear. Patients with multiple concurrent injuries (clavicle + rib fractures, or Chance fracture + bowel repair) face compounding timelines where one injury's recovery constraints overlap with another's. The following phases apply to moderate-to-severe seatbelt injury presentations:
Recovery Phases
How Insurance Companies Attack Seatbelt Injury Claims
Seatbelt injuries create a specific litigation environment that insurance adjusters and defense medical examiners exploit with practiced precision. Knowing the playbook in advance protects your claim.
Named Insurance Defense Tactics
Tactic 1: "You weren't injured because you were wearing your belt."
The adjuster argues that a properly worn seatbelt should prevent injury, implying your injuries are fabricated or exaggerated. The counter: seatbelt syndrome is a documented clinical entity. Peer-reviewed trauma literature confirms that three-point belts directly cause clavicle fractures, sternal fractures, and hollow viscus injuries. A seatbelt sign is objective evidence of the force magnitude. The belt saved your life; it also caused documented anatomical damage.
Tactic 2: "These are just pre-existing degenerative changes."
An IME physician reviews your imaging and attributes your Chance fracture, disc herniation, or rib findings to age-related degeneration or prior conditions. The counter: temporal proximity, the mechanism, and the imaging pattern are decisive. A Chance fracture at L2 is not a degenerative finding. It has a specific morphology, a specific force vector, and a specific correlation with seatbelt use documented in the American Journal of Roentgenology. The fracture did not exist before the crash, and the crash is on record.
Tactic 3: "Soft tissue only, minimal injury."
The adjuster dismisses your claim as strain or sprain with low medical documentation. The counter: if CT imaging was performed and shows sternal fractures, multiple rib fractures, or a Chance fracture, these are not soft-tissue injuries. Request copies of all imaging and imaging reports from every facility you visited. If CT was not performed and your symptoms are consistent with more serious injury, return for formal imaging. Documented bony injury cannot be characterized as "soft tissue."
Tactic 4: Surveillance and Independent Medical Examination (IME).
The defense retains a physician for an IME at a time and location of their choosing. IME physicians selected by insurance carriers have documented rates of "no injury" findings well above those of treating physicians. Your treating physician's records, imaging reports, and documented functional limitations are the strongest defense against a biased IME opinion.
Kentucky Law and Your Rights After a Seatbelt Injury
Kentucky has specific statutory and common-law rules that directly affect seatbelt injury claims. Understanding them prevents you from being misled by insurance representatives.
KRS 189.125: Mandatory Seatbelt Law. Kentucky Revised Statute 189.125 makes seatbelt use mandatory for all occupants. However, the statute explicitly provides that failure to wear a seatbelt is not negligence per se and that seatbelt non-use evidence is admissible only to mitigate damages, not to establish fault for the accident itself. The statute confirms: using your seatbelt as required (and being injured by it) does not impair your right to recover from the at-fault driver.
KRS 304.39-060: Kentucky's PIP Tort Threshold. KRS 304.39-060 sets the threshold for bringing a tort claim against an at-fault driver. Seatbelt injuries that involve fractures (clavicle, sternum, ribs, lumbar Chance fracture) generally satisfy the threshold requirements based on injury severity. Soft-tissue-only presentations may require documented medical expenses exceeding threshold amounts. An attorney can evaluate which threshold your injuries satisfy.
Comparative Fault and Seatbelt Non-Use. Under Kentucky's pure comparative fault system, KRS 189.125 permits the defense to introduce evidence of seatbelt non-use to mitigate (reduce) the damages awarded, not to eliminate the claim entirely. Even if you were not wearing a belt, Kentucky's comparative fault system means you can still recover compensation reduced by your assigned percentage of fault. There is no threshold at which you are entirely barred.
What to Do After a Seatbelt Injury in Kentucky
- Photograph the seatbelt sign (bruising or abrasions) immediately and at 24–48 hour intervals before it fades
- Request all medical records and imaging from every facility including the ER, urgent care, and any follow-up imaging centers
- Do not provide a recorded statement to the at-fault driver's insurance company before speaking with an attorney
- Keep a daily log of pain, limitations, and how your injuries affect work and daily activities
- Preserve the vehicle if possible for inspection of seatbelt condition and deployment records
Frequently Asked Questions: Seatbelt Injuries
What is seatbelt syndrome? +
Seatbelt syndrome is a clinical pattern first described in 1962 that combines the visible seatbelt sign (bruising across the abdomen or chest), intestinal perforation or mesenteric tear, and lumbar Chance fracture. It results from lap-belt restraint forcing the spine into extreme flexion during a high-force collision. BMJ Case Reports documents the complete syndrome including bowel perforations and lumbar fracture-dislocations from lap-belt use in modern vehicles.
Does a seatbelt mark mean I am seriously injured? +
A visible seatbelt sign (bruise or abrasion) correlates with underlying injury in approximately 30% of cases, according to research published in RadioGraphics. A mark does not guarantee serious injury, but it does indicate that sufficient force was applied to the tissue beneath the belt to cause contusion. Any seatbelt sign on the abdomen combined with pain or tenderness warrants CT imaging, per published trauma guidelines. Do not dismiss the mark as minor without a complete evaluation.
Can a seatbelt cause a Chance fracture? +
Yes. The Chance fracture was originally described in 1948 in patients wearing lap seat belts during vehicle accidents. The lap belt acts as the axis of rotation, subjecting the posterior spinal elements at L1–L3 to tension and flexion-distraction forces. The American Journal of Roentgenology documents that Chance-type fractures occur in motor vehicle crashes with seat belt use as the predominant mechanism and are associated with intra-abdominal injury in 40% of cases. CT with sagittal reconstructions is required to identify the horizontal fracture plane.
What imaging is needed after a seatbelt injury? +
A complete workup for seatbelt injury includes: (1) chest X-ray AP and lateral views for rib, sternal, and clavicle fractures; (2) FAST exam (bedside ultrasound) for free abdominal fluid; (3) CT chest/abdomen/pelvis with IV contrast for solid and hollow organ injury and vascular injury; (4) lumbar CT with sagittal and coronal reconstructions for Chance fracture identification; and (5) MRI when ligamentous injury or neurological symptoms persist despite negative CT. Per EAST practice management guidelines, a negative FAST does not exclude bowel injury and should be followed by CT in high-risk patients.
How long does a Chance fracture take to heal? +
Stable Chance fractures (pure osseous, no neurological deficit) treated with a TLSO brace typically achieve bony healing at 10–12 weeks with gradual return to activity at 3–4 months. Unstable fractures requiring posterior pedicle screw and rod fixation involve a 6–12 week post-surgical rehabilitation phase, with return to unrestricted activity at 4–6 months. According to AO Foundation surgical protocols, patients with intact neurological status begin walking within 2 days of surgery and are followed with serial X-rays at 6 weeks, 3 months, 6 months, and 1 year.
Does Kentucky require seatbelt use? +
Yes. KRS 189.125 makes seatbelt use mandatory for all occupants in Kentucky. Law enforcement may stop and cite drivers for seatbelt non-compliance. The statute does not, however, create negligence per se from non-use in civil injury cases. Evidence of non-use is admissible only to mitigate damages, not to bar a claim entirely.
Can I make a claim if I was not wearing a seatbelt? +
Yes. Kentucky follows a pure comparative fault system. Seatbelt non-use may reduce the damages you recover based on an assigned percentage of fault, but it does not bar your claim entirely. Under KRS 189.125, the defense must demonstrate a causal connection between non-use and the specific injuries sustained. You can still recover for injuries you would have suffered regardless of belt use, and your claim remains viable even if your fault percentage is high. An attorney can evaluate how this applies to your specific injuries and circumstances.
Is a sternal fracture from a seatbelt considered serious? +
A sternal fracture is a serious injury. It indicates that significant force was transmitted through the sash strap to the sternum, which also means adjacent structures (heart, aorta, ribs) were exposed to similar forces. Research in RadioGraphics documents that chest abrasions from seatbelt contact are specifically associated with sternal fractures, rib fractures, cardiac contusion, and thoracic aortic injury. CT imaging of the chest is required to evaluate the full injury pattern. A sternal fracture cannot be characterized as a minor or soft-tissue injury.
How do I document my seatbelt injury for my case? +
Documentation starts in the ER: ensure your treating nurse and physician note the seatbelt sign in your medical records. Photograph the bruising and abrasions yourself at multiple time points over the first week as the pattern develops. Obtain all imaging reports (X-ray, CT, MRI) and retain every record from every facility. Keep a daily journal of your symptoms, activity limitations, and the effect on your work. Preserve photographs of your vehicle showing belt deployment, seat position, and any structural damage. This contemporaneous documentation is far more persuasive than retrospective descriptions months later.

